Low FODMAP Diet
What Does FODMAP Mean?
FODMAP is an acronym describing specific types of short-chain carbohydrates (sugars):
F - Fermentable
O - Oligosaccharides (oligo = few sugar molecules)
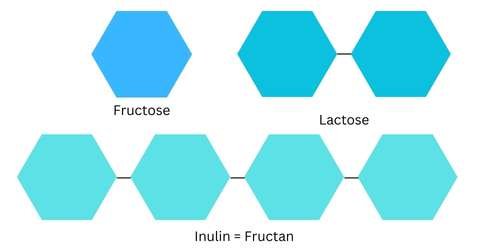
D - Disaccharides (di = two sugar molecules)
M - Monosaccharides (mono = one sugar molecule)
A - And
P - Polyols (poly = many; polyols are sugar alcohols — not the alcohol beverage kind)
The terms mono, di, and oligo refer to how many sugar molecules are linked together.
These groups include:
Oligosaccharides: Fructans (FOS), Galacto-oligosaccharides (GOS)
Disaccharides: Lactose
Monosaccharides: Excess fructose
Polyols: Sorbitol and mannitol (naturally occurring), and xylitol and maltitol (commonly used as additives)
FODMAPs are naturally present in many nutritious foods and can be part of a healthy diet.
Why Do FODMAPs Cause Symptoms?
FODMAPs are poorly absorbed in the small intestine, allowing them to reach the large intestine, where two processes occur:
Water is drawn into the intestine, increasing bowel volume and pressure.
Gut bacteria ferment these carbohydrates, producing gas.
These are normal physiological responses. However, in people with sensitive digestive systems, such as those with irritable bowel syndrome (IBS), these processes can lead to:
Bloating
Abdominal distension
Excess gas
Constipation and/or diarrhoea
How Can A Dietitian Help With IBS?
A dietitian that is trained in IBS management will:
Take a comprehensive, whole-person approach
Ensure you have a confirmed IBS diagnosis from a doctor
Identify any red flag symptoms and refer you for medical assessment if needed
Discuss bowel habits openly and professionally
Recognise that FODMAPs are not the only dietary triggers
Consider non-diet factors such as stress, mental health, the gut-brain axis, medications, hormones, menstruation, and pelvic floor function
Prioritise the least restrictive approach possible
Ensure your diet remains nutritionally balanced and sustainable
What is the Low FODMAP Diet?
The low FODMAP diet was developed in Australia by researchers at Monash University. It is a three-phase process designed to identify an individual’s sensitivity to FODMAPs.
Phase 1: FODMAP Restriction (2-6 weeks)
High-FODMAP foods are temporarily replaced with low-FODMAP alternatives to determine whether symptoms improve.
Phase 2: FODMAP Reintroduction (6-8 weeks)
Each FODMAP group is systematically reintroduced to identify specific triggers and tolerance levels.
Phase 3: FODMAP Personalisation (long-term)
This phase focuses on expanding the diet to include as many tolerated foods as possible while only limiting those that consistently trigger symptoms. Regular re-testing is important, as tolerance can change over time.
What is the Evidence for a low FODMAP Diet?
Research shows that the low FODMAP diet improves symptoms in approximately 75% of people with IBS.
How Long Should You Follow the Low FODMAP Diet?
Phase 1 should not exceed 6 weeks
Phase 2 should be limited to 6-8 weeks
Phase 3 is a personalised, long-term approach
If symptoms do not improve within two weeks of starting Phase 1, it is recommended to seek support from a FODMAP-trained dietitian
Are There Any Risks With the Low FODMAP Diet?
Any restrictive diet carries potential risks if not implemented under supervision.
FODMAP-containing foods often provide important nutrients, including prebiotic fibres that support beneficial gut bacteria. These bacteria produce compounds that support overall gut and metabolic health.
Over-restriction can also:
Reduce dietary variety
Increase stress around food
Make social eating and meal planning more difficult
Negatively impact mental health
Increase risk of disordered eating patterns
Lead to developing an eating disorder
For these reasons, the goal is always to follow the least restrictive diet necessary to manage symptoms.
Examples of High FODMAP Foods
Fructans (FOS): Onion, garlic, wheat, rye, pasta, dates, dried figs, artichoke
Galacto-oligosaccharides (GOS): Baked beans, lentils, chickpeas, cashews, green peas
Sorbitol: Apple, pear, avocado, lychee, sugar-free lollies
Mannitol: Mushrooms, cauliflower, celery
Excess fructose: Apple, mango, watermelon, honey, fruit juice
Lactose: Milk, yoghurt, custard, ice-cream
Examples of Low FODMAP Foods
Vegetables: Carrots, potatoes, corn, green beans
Fruits: Blueberries, strawberries, kiwi fruit
Protein: Meat, poultry, seafood, eggs, firm tofu, tempeh
Grains: Rice, oats, polenta, corn tortillas, spelt sourdough
Dairy: Hard cheeses, lactose-free dairy, cream
Fats: Oils, butter
Nuts: Almonds, peanuts, walnuts
Drinks: Tea, coffee